Low Back Pain-Part 1
According to many physical therapy experts, low back pain (LBP) is very common. Thoughts are that a majority of people will experience LBP at some time in their lives.
An episode of LBP can be unpleasant and it is common to experience fear and worry as a response to this type of pain. If you are not sure what to do for your LBP, then you should consult with your local pain clinic for pain relief services, especially if you’re looking for a reputable clinic for vascular treatment. Or go to your local hospital where an ER technician and pain doctor can assist you.
The good news is that your back is a strong structure and with helpful advice, episodes of low back pain are manageable. By also visiting online sites, you will see some physiotherapy treatments. Try to browse a good wellness website like https://qckinetix.com/kansas-city/ to best help treat your lower back pain and more.
Unfortunately there are many negative beliefs that exist in regards to LBP. This can make recovery difficult and these unhelpful beliefs can present a challenge for both the patient and the clinician.
Recent research highlights the current best practice guidelines for the management of LBP. If we can look to manage LBP in line with the current evidence, we hope to better manage these acute episodes and prevent episodes of LBP from persisting.
In a series of posts, our aim is to discuss LBP and current guidelines for the management of LBP in light of the current evidence.
What is the cause of my LBP?
Let’s begin by discussing some of the potential causes of LBP.
Non specific LBP
Most LBP is diagnosed as “non specific” in that there is no specific cause we can identify. This may account for up to 90% of cases. However, just because we are unable to identify a specific cause, this does not mean the structures of your spine are not painful.
Most episodes of acute non specific LBP can be thought of like a minor sprain. The back and its structures become “sensitised” rather than damaged.
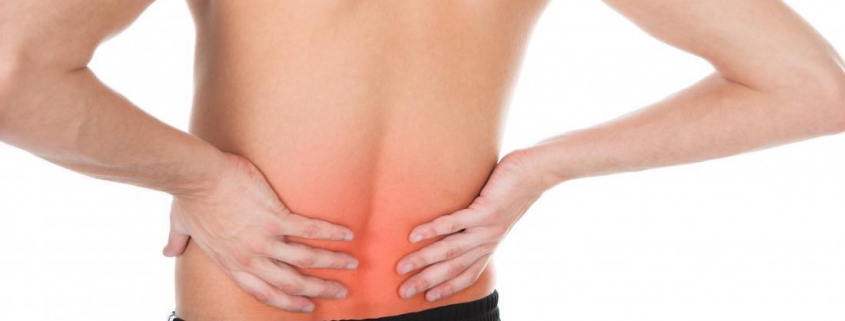
Symptoms include pain in the low back region and there may be associated pain in the legs. The low back may feel painful to touch and sometimes we have difficulty moving like we normally would.
Sometimes we know when we first felt our LBP start, and other times it may be more difficult to pin point the exact incident.
Interestingly, there is evidence that lifestyle factors such as stress may also lead to episodes of LBP.
Remember, non specific LBP may still be very painful.
Specific LBP
Specific LBP is termed when there is an anatomical or pathological cause for the LBP.
Only a small percentage of people will have a “specific” cause of their LBP, and this is currently estimated at 5-10%.
Specific LBP-Neurological
- Radicular pain or radiculopathy indicates nerve root involvement, most commonly caused by inflammation or disc changes which will require herniated disc treatment. Symptoms may include nerve pain, leg pain worse than back pain, leg pain with coughing or sneezing, weakness and/or loss of sensation in part of the leg.
- Spinal stenosis is usually caused by narrowing of the spinal canal. Symptoms include pain that is often severe in one or both legs, pain that worsens with walking or standing, easing with sitting.
- Cauda Equina Syndrome refers to damage of the bundle of spinal nerves at the bottom of the spine. Important symptoms to look out for here include loss of bowel and bladder control, and changes to sensation in that area. Treatment for this includes minimally invasive spine surgery, which is a proven safe and effective spinal treatment.
The above cases are more rare, however, these cases may require more specific medical attention, so it is important to be aware of some of the more serious signs and symptoms.
Specific LBP-Pathological
Serious pathology is estimated in 1-2% of the population, so again these causes are far more rare. Specific pathologies may include:
- Spinal Fracture
- Inflammatory disease of the spine
- Malignancy
- Infections of the spine
Symptoms such as constant severe back pain, night pain, morning stiffness and past history of malignancy are important things to look out for here.
The screening process for patients with LBP aims to assist in diagnosing a specific vs a non specific cause.
Where a specific cause to the LBP is suspected, medical imaging may be required to assist in a diagnosis.
Medical imaging, however, in the absence of these specific signs and symptoms is generally not warranted. (This will be discussed in more detail in our next post).
Should I see a Physiotherapist for my LBP?
You may find that your LBP is short lasting and goes away on its own or you may decide to seek care to help manage your symptoms and get a much needed back pain relief.
A large proportion of LBP episodes are acute (lasting 6 weeks or less) and will often go away on their own. Sometimes your episode may only last 1-2 weeks, or a few days.
The decision to visit a physical therapy center to seek help with management for your LBP may depend on things such as your level of pain and how it is affecting your daily life.
If you decide to seek further advice, a physiotherapy specialist can help. You may ask about getting a deep tissue massage to relieve your lower back and muscle pain. An Assisted Stretch Therapist can also offer massage options that can provide pain relief.
Your physiotherapist will usually do an initial clinical examination in order to guide them with your management. In some instances you may also be asked to fill out a questionnaire about your pain. This also helps to guide the clinician with your management.
Current guidelines encourage a “whole person approach” to the management of LBP. An emphasis on clear communications and helpful messages early on to help reduce fear and worry are important. It is important to keep moving and keep active where possible. These and more current guidelines for the management of acute non specific LBP will be discussed in more detail in another post.
Thanks for reading.
References:
Bunzli S et al, Journal of Orthopaedic & Sports Physical Therapy 2017 https://www.ncbi.nlm.nih.gov/pubmed/28704621
O’Sullivan P et al, Journal of Orthopaedic & Sports Physical Therapy 2016 https://www.ncbi.nlm.nih.gov/pubmed/27802794
O’Sullivan P and Lin I, Pain Management Today 2014 http://www.pain-ed.com/wp-content/uploads/2014/02/Osullivan-and-Lin-Pain-management-today-2014.pdf
Hartvigsen J et al, Lancet 2018 https://www.ncbi.nlm.nih.gov/pubmed/29573870
Foster NE et al, Lancet 2018 https://www.ncbi.nlm.nih.gov/pubmed/29573872
Disclaimer: this information is for your education/information and should not be considered medical/physiotherapy advice regarding diagnosis or treatment recommendations.

Leave a Reply
Want to join the discussion?Feel free to contribute!